- Bengaluru -Vijayanagar
- +91 80 2340 1200
- |
- Bengaluru -HSR Layout
- +91 89708 22333
- |
- Kochi
- +91 74061 88800


At Cutis, you’re in safe hands with Dr. B.S. Chandrashekar and our team of specialists. Just fill out the form, and we’ll get in touch to confirm your visit.




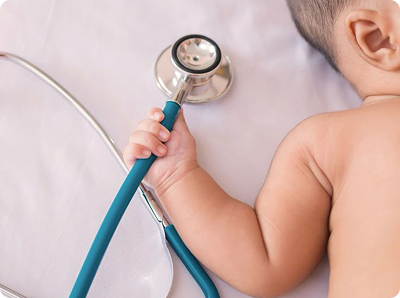






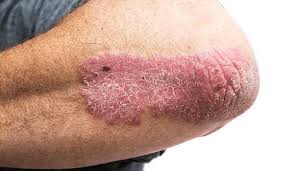
Introduction Psoriasis is a chronic, autoimmune inflammatory skin condition affecting
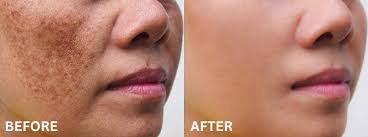
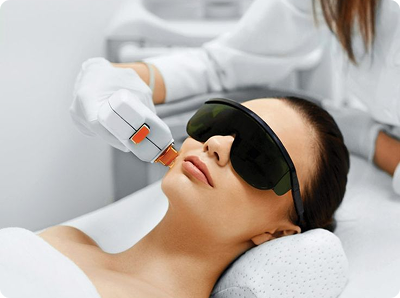
Introduction Melasma is a chronic hyperpigmentation disorder affecting millions worldwide,
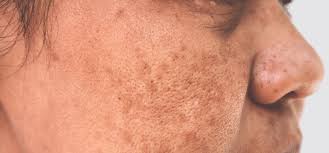
Introduction Pigmentation disorders are among the most common and emotionally